The Adrenal-Gut-Immune Triangle: Why Treating One Without the Others Keeps You Stuck
There's a patient I think about a lot. She had tried everything. The elimination diets, the probiotics, the gut protocols. She'd had a stool analysis done. She'd cut out gluten, dairy, and everything else that gets blamed on Instagram. She was still exhausted. Still getting ill. Still stuck. The reason? She'd been treating one corner of a triangle while the other two corners were pulling in the opposite direction.
Last week I talked about the gut-immune axis — the reason why 70% of your immune cells live in and around your gut, and why gut health is inseparable from immune function. If you missed it, it's worth reading first, because this week builds directly on it.
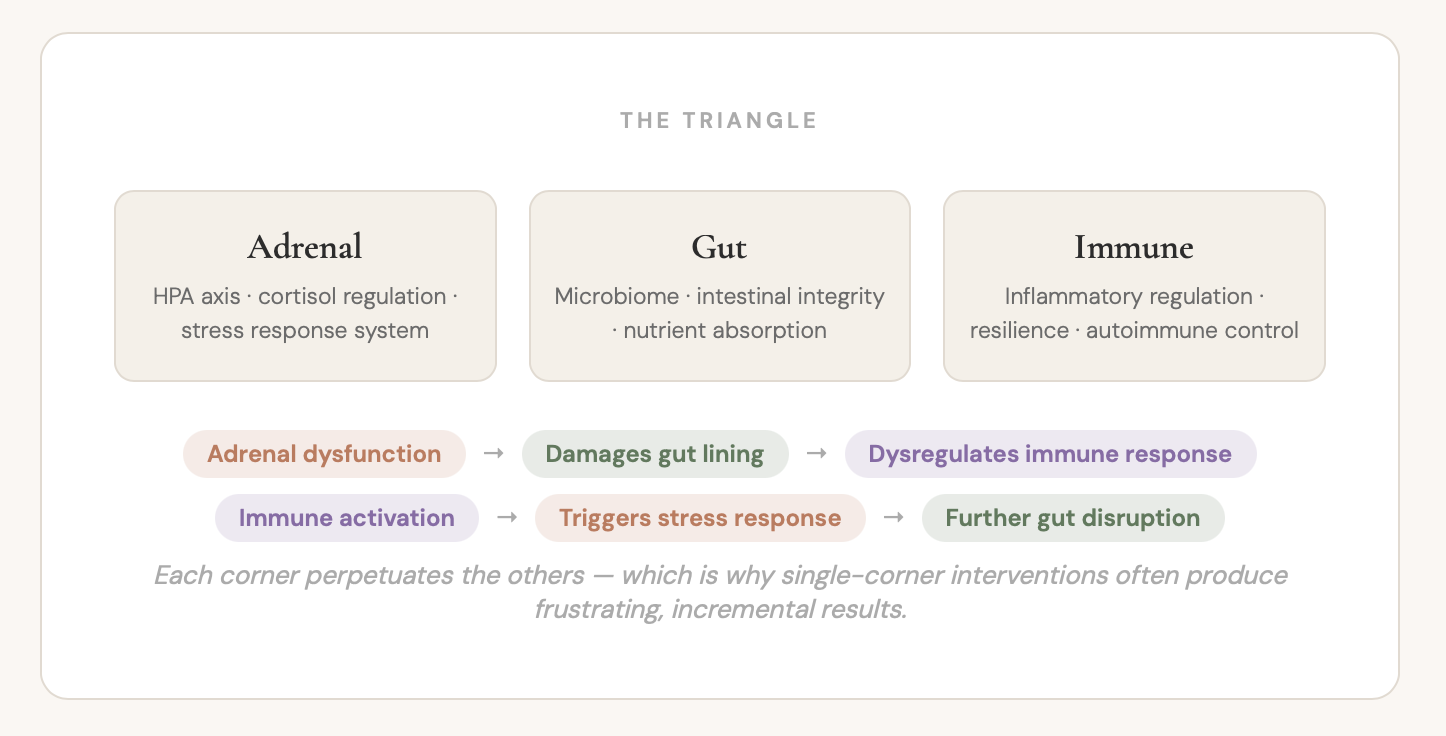
This week I want to add a third corner to the picture: your adrenal system. Because in clinical practice, I rarely see gut-immune problems that aren't also adrenal problems. And I rarely see adrenal problems that aren't also gut-immune problems. They are a triangle. And the triangle is self-reinforcing in ways that explain why so many people feel stuck even when they're doing things right.
The Adrenal System: What It Actually Does
Your adrenal glands are small — they sit on top of your kidneys — but they produce some of the most systemically important hormones in the body. Cortisol is the most well known, but they also produce DHEA, aldosterone, and adrenaline. Together, these shape your energy levels, your immune regulation, your blood pressure, your blood sugar response, and your sleep-wake cycle.
The adrenal system doesn't just respond to acute stress — it's the infrastructure your body uses to maintain function under pressure. And the problem in modern life is that it rarely gets adequate recovery time. The stress isn't the kind that resolves — a threat that passes, a crisis that ends. It's low-level, persistent, and relentless. Deadlines, difficult relationships, financial pressure, the physiological burden of poor sleep and ultra-processed food and too much caffeine and not enough downtime.
Over time, under that kind of load, the HPA axis — the hypothalamic-pituitary-adrenal system that coordinates the stress response — begins to dysregulate. Not fail. Not collapse. Dysregulate. The cortisol pattern becomes abnormal. The morning spike that should energise you becomes blunted. The evening low that should allow you to wind down becomes elevated. Energy becomes unpredictable. Sleep becomes disrupted. And the immune system, which depends on appropriate cortisol signalling to regulate its activity, starts to behave in ways it shouldn't.
How Chronic Stress Breaks the Gut-Immune Relationship
This is the piece that connects everything. Cortisol has a direct, physiological effect on the gut. In acute stress, it redirects resources away from digestion (you don't need to be digesting food when you're running from a threat). In chronic stress, those effects become sustained and damaging.
Cortisol directly increases intestinal permeability.The tight junctions between gut cells — which are supposed to keep the gut contents in the gut — become more porous under sustained cortisol exposure. This is measurable. It's not a hypothesis.
Cortisol disrupts the microbiome.Beneficial bacterial populations decline under chronic stress. Pathogenic bacteria and yeasts get more of a foothold. Dysbiosis is not just a dietary problem — it's a stress response problem.
Cortisol suppresses secretory IgA— the immune antibody that lines your gut and protects the barrier. Lower sIgA means lower gut immune defence. More reactivity to food proteins, more vulnerability to pathogens.
So when someone comes to me having tried every gut protocol and still seeing limited results, the first question I ask is: what is the adrenal picture? Because if cortisol dysregulation is actively degrading the gut environment, gut interventions alone will always produce partial results. You're trying to repair something that's being continuously damaged.
““Why treating one without the others keeps you stuck — and why the order of intervention matters as much as the intervention itself.””
The Triangle Is Self-Reinforcing
Here's the part that explains why so many people with these patterns feel like they're going in circles.
Stress damages the gut. A damaged gut increases intestinal permeability. Permeability means toxins, undigested food proteins and bacterial components enter the bloodstream. The immune system mounts a response. Inflammatory signalling activates the stress response further. More cortisol. More gut damage. More immune activation.
The triangle feeds itself. And if you're only ever addressing one corner — taking probiotics, or cutting out foods, or doing breathwork — you're not breaking the cycle. You're managing one corner while the other two continue to perpetuate it.
A PATTERN I SEE CONSTANTLY
Someone comes to me who has done everything. They've tried every elimination diet. They've been painstakingly consistent with supplements. They've worked with three different nutritional therapists. And they still feel awful.
When I look at their adrenal picture — a four-point salivary cortisol curve across the day — the pattern tells the story. The morning spike is flat when it should be high. The afternoon is elevated when it should be declining. The evening is still elevated when it should be low. Their nervous system isn't in a recovery pattern at any point during the day.
Every gut intervention they've done has been working against this background cortisol dysregulation. The gut can't repair under those conditions. The immune system can't recalibrate. We need to address the adrenal picture first — or at least simultaneously — for everything else to land.
What Working All Three Corners Looks Like
In functional medicine practice, addressing the triangle simultaneously means something specific for each corner.
THE ADRENAL CORNER
Blood sugar stabilisation — cortisol spikes every time blood sugar drops, so eating in a way that prevents blood sugar instability directly reduces adrenal load
Nutrient replenishment — magnesium, vitamin C, B5 (pantothenic acid), and zinc are specifically depleted by chronic HPA activation and needed for normal cortisol production
Sleep architecture — not just duration, but the structure of sleep, which is when HPA axis recovery actually happens
Reducing input demand — not eliminating stress, but identifying the most significant physiological stressors and reducing them where possible
THE GUT CORNER
Remove the main inflammatory triggers — dietary and otherwise — that are actively driving gut inflammation
Repair the gut lining with targeted nutrients: L-glutamine, zinc carnosine, collagen, omega-3s
Rebuild the microbiome with diverse fibre, fermented foods, and where appropriate, targeted probiotic support
Support digestive function — enzymes, stomach acid — because dysbiosis and stress often reduce digestive capacity
THE IMMUNE CORNER
Reduce the inflammatory load directly — omega-3 fatty acids, dietary antioxidants, anti-inflammatory nutrition
Identify any specific immune drivers — food sensitivities, latent infections, environmental triggers — that are keeping immune activation elevated
Support the regulatory side of immune function, not just the active side — this is where the gut work and the adrenal work overlap most significantly
The Blood Tests Nobody Orders
One of the things I've been covering in my reels this week is the gap between what GPs routinely test and what functional medicine looks at. For the adrenal-gut-immune triangle, the markers that matter most are almost never included in a standard panel.
WHAT FUNCTIONAL MEDICINE LOOKS AT
4-Point Salivary Cortisol
Tests cortisol at waking, 30–60 mins post-waking, afternoon, and evening. This gives the full diurnal pattern — not just whether cortisol is in range, but whether the rhythm is functional.
NHS: Not available. Single serum cortisol only tests for Addison's or Cushing's.
High-Sensitivity CRP
Standard CRP detects acute inflammation. hs-CRP detects chronic, low-grade inflammation — the kind that drives fatigue, brain fog and autoimmunity without triggering a conventional red flag.
NHS: Standard CRP only. hs-CRP not routinely included.
Full Thyroid Panel
TSH, free T4, free T3, reverse T3, and thyroid antibodies. Stress and adrenal dysfunction directly impair thyroid conversion — the picture behind "normal TSH, still symptomatic" is often here.
NHS: TSH only. Free T4 occasionally. Antibodies rarely without specialist referral.
Ferritin
Functional medicine optimal: 70–100 mcg/L minimum. A ferritin of 16 mcg/L is technically "normal" by NHS criteria and represents near-depletion of iron stores, explaining fatigue, hair loss, and poor cognitive function.
Understanding these markers doesn't require a functional medicine practitioner to interpret them — it requires knowing what to ask for and what "optimal" looks like, as opposed to what "not diagnosable" looks like. These are very different things.
Start understanding your own triangle
The 7 Day Reset is built around addressing all three corners simultaneously — because that's the only way to break the cycle.